Evaluation plays a critical role in healthcare improvement by ensuring that interventions and programs deliver intended outcomes. It provides evidence to measure impact, optimize resources, and support continuous learning. Selecting the right evaluation methodology is crucial for making informed decisions and improving clinical practices.
The purpose of evaluation
Evaluation serves multiple functions in healthcare. It assesses the effectiveness of interventions, ensuring they achieve desired outcomes while helping to refine, scale, or discontinue initiatives. Decision-makers rely on evaluation to optimize resource allocation, ensuring investments yield the highest value for patients and healthcare systems. Additionally, evaluation fosters learning and adaptation by identifying successes and areas for improvement
Key evaluation approaches
1. Process evaluation
Process evaluation focuses on how an intervention is implemented and what factors influence success or failure. It examines whether an initiative is delivered as intended, explores stakeholder experiences, and identifies systemic challenges. By understanding these elements, organizations can refine their approaches and improve future implementations.
Case example: Telemedicine
In evaluating digital tools and telemedicine solutions, we conducted a process evaluation to understand both patient and healthcare provider experiences. We interviewed patients about accessibility, ease of use, and perceived benefits and barriers. Similarly, healthcare professionals shared insights into workflow integration and efficiency changes.
A mixed-methods approach combined qualitative interviews with register data on app usage and telemedicine adoption. We tracked changes in usage patterns to determine whether patients adopted new app-based modes of contact and dialogue. We assessed whether self-booking reduced cancellations. Finally, we measured how redesigned patient pathways affected treatment burden by looking at contact patterns for individual patients over time. By integrating these findings, we provided actionable recommendations to optimize digital health solutions during the process of implementation.
2. Realistic evaluation
Realistic evaluation is an evaluation methodology that seeks to determine what works, for whom, and under what conditions. Using the Theory of Change (ToC) framework uncovers causal mechanisms, assesses contextual influences, and provides guidance on how interventions should be adapted. This approach is particularly valuable for complex interventions when it’s not enough to determine whether interventions are effective but also how and why.
Case example: Testing and scaling technology
A mental health program aimed at improving access to digital support tools and structured care was evaluated using a realistic evaluation approach. Given the complexity of the intervention—including technology adoption, engagement of vulnerable users, and integration with public services—it was crucial to understand both implementation factors and the actual effect of the program.
A mixed-methods design combined qualitative and quantitative approaches. Interviews with project managers and partners assessed implementation strategies and barriers, while participant interviews explored experiences and perceived value. A survey using validated patient-reported outcome measures (PROMs) tracked changes in mental health status over time to determine whether the efforts yielded positive effects. To determine impact, a cost-effectiveness analysis compared program costs to improvements in well-being.
By integrating these methods, the evaluation identified key mechanisms for success, such as effective technology integration and tailored support for vulnerable users. Findings guided adaptation and scaling while providing strong evidence for decision-makers.
3. Health economic evaluation
Efficient use of healthcare resources is vital, making economic evaluation an essential component of decision-making. Cost-effectiveness analysis (CEA) compares costs and clinical outcomes to identify the most efficient interventions. Cost-utility analysis (CUA) incorporates patient preferences, measuring outcomes in quality-adjusted life years (QALYs), while cost-benefit analysis (CBA) quantifies both costs and benefits in monetary terms to assess overall value. These approaches ensure that financial sustainability aligns with clinical effectiveness.
Case example: Testing and scaling technology
A cost-effectiveness analysis was conducted to evaluate an innovative new insulin pump. We conducted a comprehensive analysis to assess both clinical and economic outcomes. We focused on key factors such as improved blood sugar regulation, reduced episodes of hypoglycemia, and long-term impacts on patients’ quality of life. Additionally, we examined the potential economic benefits of the new technology in relation to existing diabetes treatments, considering both the direct and indirect costs for patients and healthcare systems. By integrating economic evaluation methods, we identified key drivers of cost-efficiency, such as optimized resource allocation and improved patient outcomes. The findings supported data-driven decision-making, ensuring that investments in healthcare interventions deliver maximum value while maintaining clinical effectiveness.
4. Evaluating public-private partnerships
Assessing the impact of PPPs in healthcare requires a structured framework. Governance and accountability must be examined to ensure clarity in roles and responsibilities. Financial sustainability is equally important, as cost-sharing models must be viable in the long run. Performance metrics should measure service quality, patient outcomes, and efficiency gains. Lastly, stakeholder satisfaction is a key indicator, providing insights from public institutions, private partners, and patients.
Case example: PPP for new health tech solutions
We have developed a framework for assessing the impact of PPPs in healthcare through a structured framework based on Theory of Change (ToC) and key performance indicators (KPIs) that enables us to track progress and long-term impact.
In our experience a comprehensive PPP evaluation framework includes:
- Establishing a joint platform: Creating a neutral space where partners define shared goals and align expectations.
- Building trust and collaboration: Developing relational strategies, transparency, and mutual benefits to sustain long-term cooperation.
- Pilot testing and scaling: Implementing small-scale projects to test feasibility before expanding successful initiatives.
- Measuring impact and sustainability: Using validated KPIs such as health improvements, economic benefits, and governance indicators to track long-term outcomes.
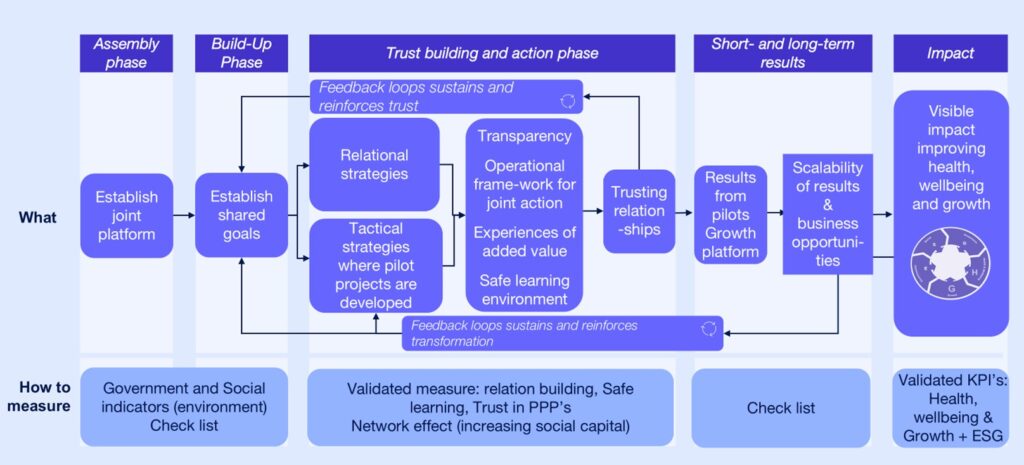
Below is a practical example of a PPP evaluation approach based on the Lighthouse Model, which is a growth platform. The Lighthouse involves all major stakeholders within life science, and it provides an infrastructure for collaboration on developing new health tech solutions across different phases of a large-scale PPP. These include the assembly phase, build-up phase, trust building and action phase, short and midterm results, and long-term impact. For each phase we have developed measures to track progress, results, and long-term impact.
Conclusion
Evaluation is more than a technical exercise—it is a strategic necessity that shapes the future of healthcare. As outlined in this article, understanding why evaluation matters, how it is conducted, and what NHG’s experience brings to the table is essential for ensuring impactful, evidence-based decision-making.
By combining process evaluation, realistic evaluation, economic analysis, and structured PPP assessments, organizations can uncover what works, for whom, and under what conditions. These insights not only refine current interventions but also lay the groundwork for scalable and sustainable improvements. Through careful assessment of costs, impact, and implementation factors, evaluation helps mitigate risks, optimize resources, and maximize value for patients and stakeholders alike.
Ultimately, evaluation is not just about proving an intervention’s success—it is about continuously improving and adapting to ensure the best possible outcomes. As a public or private client, can you afford not to evaluate your solutions, interventions, and projects? Let’s get in touch if we can help you gain the insights you need to determine the right evaluation approach. Thoughtful evaluation fosters better patient care and enhances healthcare system efficiency.
Rune Puggaard, Partner, Nordic Healthcare Group Denmark
rune.puggaard@nhgdk.dk / +45 25 94 88 92
Marie-Louise Mølbak, Partner, Nordic Healthcare Group Denmark
marie-louise.molbak@nhgdk.dk
